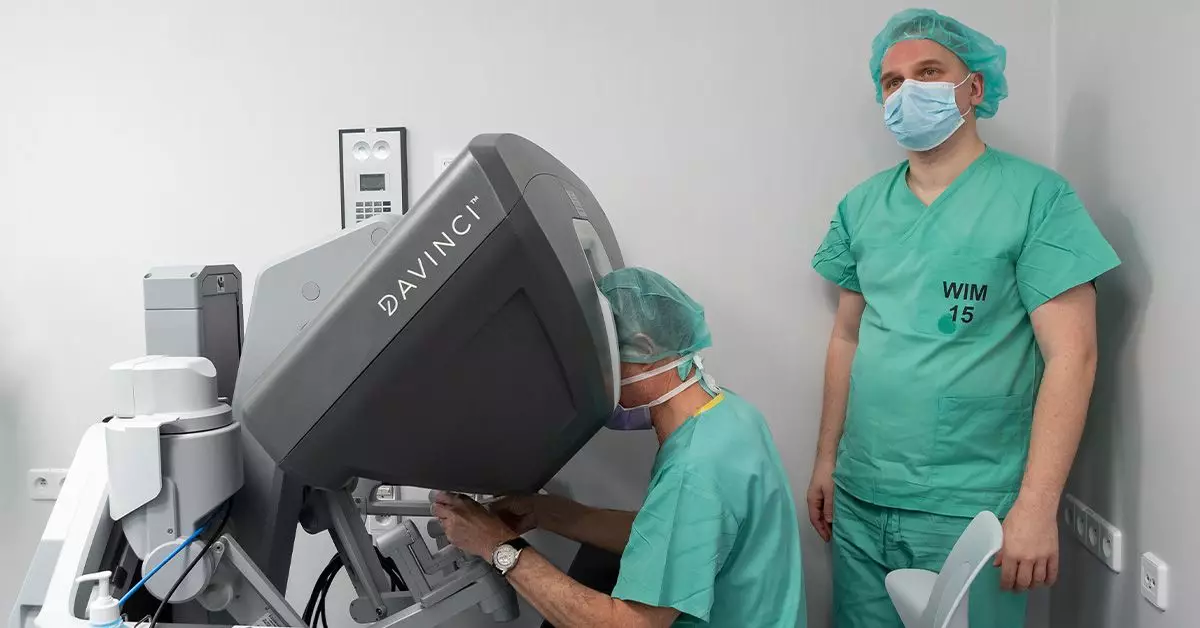
Transoral robotic surgery (TORS) has emerged as a groundbreaking technique in the realm of minimally invasive surgery, particularly for diseases and tumors associated with the head and neck. This advanced surgical method is distinguished by its ability to access the surgical site through the mouth, thus obviating the need for external incisions. This innovative approach relies on sophisticated robotic systems, like the Da Vinci Robotic System (DVRS), which empower highly trained surgeons to execute intricate procedures with enhanced precision and less trauma to the patient.
The TORS process utilizes a robotic platform equipped with articulated arms designed to replicate the dexterity of a surgeon’s hands, albeit on a much smaller scale. The central arm is integrated with a high-resolution camera that provides surgeons with a clear and magnified view of the surgical field. Simultaneously, the two lateral arms perform the surgery under the direct control of the surgeon from a console. This unique configuration allows for meticulous manipulation within the confined anatomical spaces of the throat and mouth, leading to improved surgical outcomes.
The technique received approval from the Food and Drug Administration (FDA) in 2009, primarily for specific benign tumors and early-stage cancers related to the head and neck. Over time, its application has expanded to encompass various conditions, including thyroid surgeries and neck dissections, establishing TORS as a versatile tool in the surgical arena.
A thorough review of various studies underscores the safety and efficacy of TORS. One of the notable studies conducted in 2022 involved a comprehensive comparison of TORS with nonrobotic surgical methods (NRS) as well as nonsurgical treatments (NST) for oropharyngeal cancer. The results were illuminating: TORS exhibited a significantly lower complication rate and was more successful in achieving complete tumor removal compared to its nonrobotic counterparts. Furthermore, as surgeons gained more experience with the TORS system, the outcomes continued to improve.
These findings indicate that surgical centers that perform TORS frequently—ten or more cases a year—see significantly better outcomes than those with lower volumes. Such data reinforces the importance of experience in leveraging advanced technologies like TORS.
The advantages of TORS extend beyond its primary purpose of treating tumors. As a minimally invasive technique, it is associated with several patient benefits. These include shorter hospital stays, expedited recovery periods, and a reduced risk of complications, such as excessive scarring. Moreover, patients undergoing TORS typically avoid the need for procedures such as tracheostomy, which is commonly employed in more invasive surgeries to facilitate breathing.
Nonetheless, it is vital to acknowledge that robotic surgery does carry inherent risks, such as the potential for mechanical failures or human errors during operation. Fortunately, these occurrences are rare, with a mechanical failure rate of merely 0.1% to 0.5%.
Before TORS, patients generally undergo a staging endoscopy which involves using an endoscope with a camera to visualize the tumor and assess its spread. This critical step ensures that surgeons are well-informed about the tumor’s characteristics prior to surgery. Patients are kept under general anesthesia for the procedure, monitored closely to ensure their safety.
Post-surgery, patients may require a temporary feeding tube as they navigate their return to normal swallowing functions. While recovery can vary, most individuals stay in the hospital for approximately three to ten days and usually require about six weeks before resuming work and other activities. Ongoing post-operative care is crucial, especially in monitoring for potential cancer recurrence, as well as ensuring that patients receive necessary adjunct therapies like chemotherapy or radiation when indicated.
Prospects and Future Directions
Emerging research indicates that TORS may provide more than just immediate treatment benefits; it holds the potential for favorable long-term outcomes. Multiple studies suggest that TORS leads to faster recovery, fewer hospital readmissions, and improved identification of primary tumors—all critical factors that can significantly affect a patient’s overall prognosis.
Surgeons also benefit from the enhanced dexterity and reduced fatigue provided by robotic surgery, which could result in a broader acceptance of TORS as a preferred approach in delicate head and neck procedures.
Transoral robotic surgery represents a paradigm shift in the treatment of head and neck conditions. With its impressive safety record, efficiency, and the numerous benefits it provides to both patients and surgeons, TORS is set to become a cornerstone of modern surgical practice. As the technology and techniques continue to evolve, the future of TORS looks promising for improving the lives of those affected by various head and neck challenges. Individuals diagnosed with cancer or other related conditions are encouraged to discuss the option of TORS with their healthcare providers to explore how this innovative approach can play a crucial role in their treatment journey.